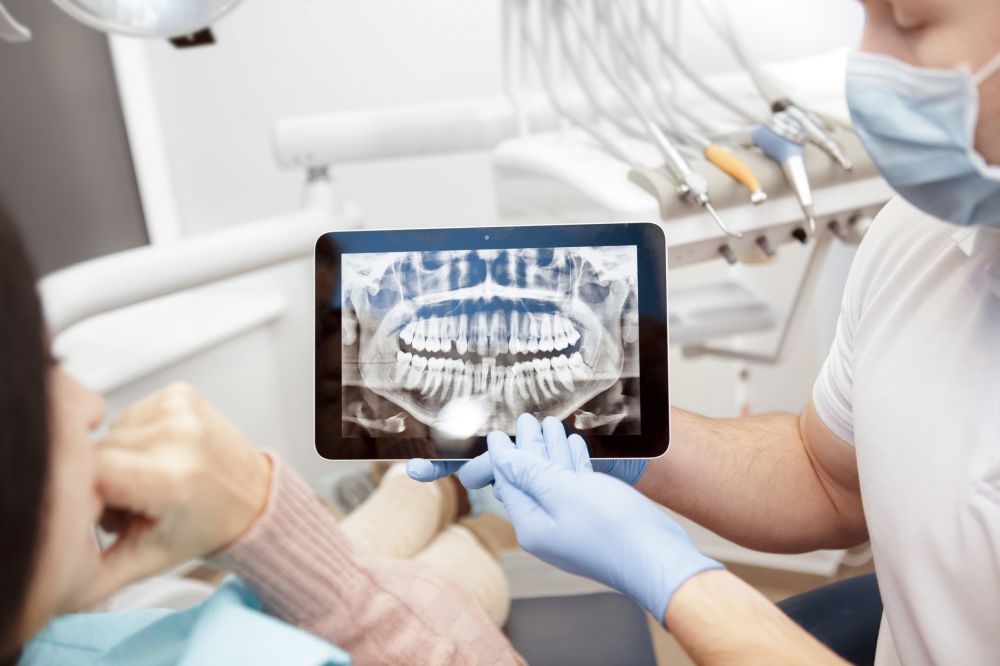
Dental diagnostics in Torrevieja
Digital Dental Diagnostics
Table of Contents
-
Consultation. General Overview.
-
Physical Diagnostic Methods.
-
Radiographic Diagnostics.
-
Microscope-Assisted Examination.
-
Photographic Documentation Protocol.
-
Plaque Disclosure Agents and Caries Detectors.
-
How Long Does the Diagnostic Process Take?
1. Consultation. General Overview
Patients often say things like "I just want a quick look" or "Why do I need an X-ray?"
It can indeed be difficult to understand why a dentist spends so much time examining the oral cavity, why they tap on the teeth, and why they request radiographs — or sometimes not just conventional X-rays, but a full cone beam computed tomography scan. That is why we would like to explain what the specialist is looking for during a consultation and why each step matters.
First, the dentist conducts a thorough medical history interview, identifying the patient's chief complaint and completing a health questionnaire that records all systemic conditions and concurrent medications. This information is essential for determining the appropriate treatment strategy and selecting suitable anaesthetic agents and dental materials.
Second, the specialist performs a comprehensive intraoral examination, documenting any observed findings: existing restorations, tooth fractures, colour changes, non-carious cervical lesions (wedge-shaped defects), gingival recession, coronal breakdown, prosthetic crowns, osseointegrated implants, signs of periodontal inflammation, supra- and subgingival calculus deposits, tooth wear (attrition, abrasion, erosion), temporomandibular joint sounds and crepitus, and headache-related symptoms. All these findings must be systematically identified and recorded.
Third, the dentist may perform physical diagnostic tests, radiographic examinations, microscope-assisted exploration, photographic documentation, and other supplementary diagnostic procedures.
2. Physical Diagnostic Methods
Following the visual examination, the specialist applies a series of clinical tests, evaluating both the nature and the intensity of the patient's responses:
-
Palpation (digital pressure applied to the teeth, gingival tissues and oral mucosa). This test helps identify areas of inflammation or tissue alteration, which may manifest as tenderness, induration or oedema. These findings provide critical diagnostic information about the condition of the oral cavity.
-
Percussion (axial and lateral tapping of the teeth). A healthy tooth will produce no pain response upon percussion, whereas pathology — such as apical periodontitis or periapical inflammation — will elicit tenderness, prompting a more detailed diagnostic evaluation.
-
Cold pulp sensitivity test (application of a chilled cotton pellet to the tooth surface). This test is used to assess pulp vitality. A tooth that responds to the cold stimulus retains a vital pulp; an absence of response indicates pulp necrosis or previous root canal treatment.
3. Radiographic Diagnostics
Radiographic imaging enables the visualisation of structures inaccessible to clinical examination: the condition of the alveolar bone, the temporomandibular joints, the internal morphology of the tooth and its roots, and other pathologies that cannot be detected by direct inspection alone.
For example, a restoration may appear clinically acceptable to the naked eye, yet a radiograph may reveal that the tooth previously underwent endodontic treatment and has since developed a periapical granuloma or cyst — a chronic inflammatory lesion at the root apex. The same image may also disclose subgingival calculus and progressive alveolar bone loss.
-
Periapical radiograph (digital intraoral radiography / RVG). Provides detailed imaging of one or two adjacent teeth. Frequently used to diagnose interproximal or hidden caries and to monitor treatment progress at each clinical stage.
-
Panoramic radiograph (OPG / dental panoramic tomography, 2D image). Provides a comprehensive view of the entire dentition, enabling assessment of alveolar bone levels, periapical pathology, root canal obturation quality, impacted or unerupted teeth, occlusal relationships, temporomandibular joints and developing tooth buds in the primary dentition. Commonly used as a baseline investigation for treatment planning.
-
Cone Beam Computed Tomography (CBCT / Dental CT, 3D imaging). Currently regarded as the most accurate diagnostic modality in clinical dentistry. Allows three-dimensional visualisation of tooth morphology, root anatomy and maxillofacial bony structures from every angle. Indicated for complex case planning, full-mouth rehabilitation and implant-supported prosthetic treatment.
-
Limited-volume CBCT for a single tooth (Endo-CBCT). This targeted radiographic modality is applied when detailed evaluation of an individual tooth is required — for example, in cases of endodontic retreatment or surgical apicoectomy. It delivers high-resolution imaging of the selected tooth, providing precise visualisation of root canal anatomy and periapical status from all projections.
-
Temporomandibular joint (TMJ) CBCT. Enables comprehensive assessment of the mandibular condyles, articular discs, ligamentous structures and surrounding tissues from all perspectives. Indicated in the diagnosis and management of temporomandibular disorders (TMD).
The more thorough the diagnostic process, the more accurate and comprehensive the treatment plan — and the more predictable the clinical outcome.
4. Microscope-Assisted Dental Examination
In certain clinical situations, it becomes necessary to identify the source of a patient's discomfort when it cannot be visualised through direct examination or conventional diagnostic methods. In such cases, the specialist employs an operating dental microscope. This instrument makes it possible to detect restoration microleakage, early-stage carious lesions, enamel microfractures, vertical root fractures, and other subtle pathological changes that would otherwise remain undetected.
5. Photographic Documentation Protocol
Clinical photography and the subsequent presentation of images to the patient provide objective, visual evidence of existing pathology, facilitate monitoring of treatment progress and enable accurate documentation of clinical outcomes. In addition, a comprehensive photographic record is indispensable in aesthetic dentistry cases, as the photographs serve as the primary reference for the dental laboratory in the fabrication of prosthetic restorations.
6. Plaque Disclosure Agents and Caries Detectors
In the diagnosis and management of periodontal diseases, gingival inflammation and bleeding on probing, as well as in oral hygiene instruction, specialist disclosure agents are routinely employed. These are available in tablet or liquid form and are applied directly to the tooth surfaces. On clinically clean areas, the dye rinses away completely upon mouthrinsing; where plaque deposits and calculus are present, they are selectively stained, clearly revealing problem areas.
Similarly, a caries-disclosing solution is applied to the tooth surface during carious tissue removal: it is washed away without trace from sound enamel and dentine, while selectively staining carious tissue, enabling the clinician to achieve a more conservative and precisely controlled excavation.
7. How Long Does the Diagnostic Process Take?
At an initial diagnostic consultation, the clinical interview, intraoral examination, completion of clinical records and, where applicable, the photographic documentation protocol typically take approximately 40 minutes. Radiographic diagnostics — including the imaging procedures themselves, digital image loading and processing, radiograph interpretation and discussion of findings with the patient — require an additional 20 minutes. In more complex cases, this timeframe may prove insufficient, and follow-up consultations will be scheduled accordingly.
At subsequent appointments — for example, post-treatment review visits or routine preventive check-ups — the time required for the diagnostic assessment is considerably reduced and may be as little as 10 to 15 minutes.
We welcome patients from Torrevieja, La Mata, Elche, Murcia, Alicante and other towns along the Costa Blanca and the Valencia Region to visit our clinic or contact us by phone.
CALL US: +(34) 638 893 141
Appointments are available by prior booking only.
Contact Information:
| Torrevieja, Pasaje Pais Vasco, edificio 1 local 4 | |
| +(34) 638 893 141 | |
| +(34) 638 893 141 | |
| apdenta@gmail.com | |
| Working hours: Mon - Fri: from 10:00 to 20:00 |